Search
- Page Path
- HOME > Search
Corrigendum
- Miscellaneous
- Corrigendum: Affiliation Correction. Development and Validation of a Risk Scoring System Derived from Meta-Analyses for Papillary Thyroid Cancer
- Sunghwan Suh, Tae Sik Goh, Yun Hak Kim, Sae-Ock Oh, Kyoungjune Pak, Ju Won Seok, In Joo Kim
- Endocrinol Metab. 2023;38(2):287. Published online April 27, 2023
- DOI: https://doi.org/10.3803/EnM.2023.202
- Corrects: Endocrinol Metab 2020;35(2):435
- 934 View
- 60 Download

Original Articles
- Clinical Study
- Development and Validation of a Risk Scoring System Derived from Meta-Analyses of Papillary Thyroid Cancer
- Sunghwan Suh, Tae Sik Goh, Yun Hak Kim, Sae-Ock Oh, Kyoungjune Pak, Ju Won Seok, In Joo Kim
- Endocrinol Metab. 2020;35(2):435-442. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.435
- Correction in: Endocrinol Metab 2023;38(2):287
- 5,589 View
- 130 Download
- 3 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The aim of this study was to develop a scoring system to stratify the risk of papillary thyroid cancer (PTC) and to select the proper management.
Methods
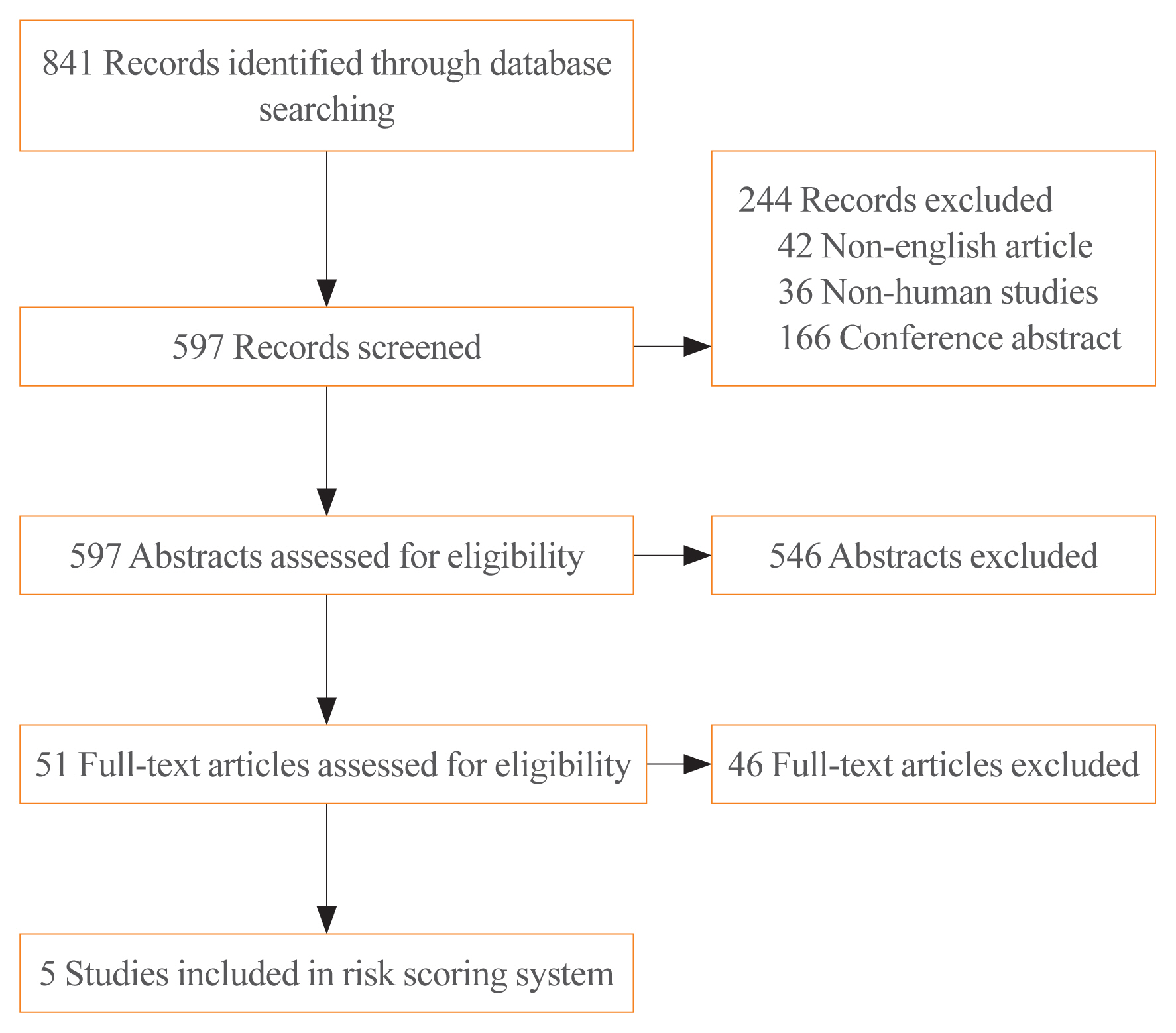
We performed a systematic search of MEDLINE and Embase. Data regarding patients’ prognoses were obtained from the included studies. Odds ratios (ORs) with statistical significance were extracted from the publications. To generate a risk scoring system (RSS), ORs were summed (RSS1), and summed after natural-logarithmic transformation (RSS2). RSS1 and RSS2 were compared to the eighth edition of the American Joint Committee on Cancer (AJCC) staging system and the 2015 American Thyroid Association (ATA) guidelines for thyroid nodules and differentiated thyroid carcinoma.
Results
Five meta-analyses were eligible for inclusion in the study. Eight variables (sex, tumour size, extrathyroidal extension, BRAF mutation, TERT mutation, histologic subtype, lymph node metastasis, and distant metastasis) were included. RSS1 was the best of the analysed models.
Conclusion
We developed and validated a new RSS derived from previous meta-analyses for patients with PTC. This RSS seems to be superior to previously published systems. -
Citations
Citations to this article as recorded by- Investigating 18F-FDG PET/CT Parameters as Prognostic Markers for Differentiated Thyroid Cancer: A Systematic Review
Hongxi Wang, Hongyuan Dai, Qianrui Li, Guohua Shen, Lei Shi, Rong Tian
Frontiers in Oncology.2021;[Epub] CrossRef - Impact of Multifocality on the Recurrence of Papillary Thyroid Carcinoma
Joohyun Woo, Hyeonkyeong Kim, Hyungju Kwon
Journal of Clinical Medicine.2021; 10(21): 5144. CrossRef
- Investigating 18F-FDG PET/CT Parameters as Prognostic Markers for Differentiated Thyroid Cancer: A Systematic Review

- Relationship between The Expressions of Sodium/Iodide Symporter and The Findings of Thallium-201 Scan in Thyroid Nodules.
- Joon Hyop An, Min Ah Na, Sang Soo Kim, Ok Nyu Kong, Ju Won Seok, Chang Hun Lee, Chang Won Lee, In Joo Kim, Yong Ki Kim
- J Korean Endocr Soc. 2004;19(2):165-174. Published online April 1, 2004
- 1,112 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The sodium/iodide symporter (NIS) has an important role in the diagnosis and treatment of well differentiated thyroid carcinoma. The relationship between the uptake of thallium- 201 scan (201Tl scan) and the expression of sodium/iodide symporter (hNIS) was studied in thyroid nodules. METHODS: Patients that had undergone operations for thyroid nodules, and who received a 201Tl scan before their operations, were investigated. Anti-NIS antibodies were used to analyze the presence and distribution of the hNIS protein by immunohistochemical staining of their thyroid tissues. RESULTS: Forty-four patients (papillary carcinoma; 18, follicular adenoma; 11, adenomatous goiter; 14, nonspecific thyroiditis; 1) 30 with no immunoreactivity and 14 with a positive reaction to the anti-NIS antibody, were included. The NIS negative patients (12/30) had no 201Tl uptake, but all others were positive on 201Tl scan, and the NIS-positive patients (13/14) had positive 201Tl uptake, with 1 negative on 201Tl scan, with significant difference (p=0.035). Of the 18 patients with a papillary thyroid carcinoma, the NIS negative patients (2/10) had no 201Tl uptake and the others were positive on 201Tl scan, but without significant difference. NIS positive patients (1/8) with a papillary thyroid carcinoma had no 201Tl uptake, and the others were positive on 201Tl scan, but without significant difference. Whether the results of NIS staining and 201Tl scan were positive or not did not affect the responses of radioactive iodine therapy in our study. CONCLUSION: These results suggest that thallium-201 uptake may be correlated with hNIS expression in thyroid nodules

- Usefulness of Thallium-201 Scintigraphy for Differentiating Benign and Malignant Thyroid Nodules in Inconclusive Cases with Fine Needle Aspiration.
- Young Sil Lee, Chang Won Lee, Mi Hwa Jang, Ju Won Seok, Seok Man Son, Seok Dong Yoo, In Joo Kim, Yong Ki Kim
- J Korean Endocr Soc. 2001;16(4-5):447-456. Published online October 1, 2001
- 1,009 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Although fine needle aspiration(FNA) is recognized as the most accurate procedure in the differential diagnosis of thyroid nodules, about 20~30% of nodules remain inconclusive in FNA. Therefore, we assessed the usefulness of Thallium-201 scintigraphy in differentiating benign from malignant thyroid nodules in patients with inconclusive diagnosis by FNA. METHODS: We studied 43 patients with inconclusive diagnosis(29 of follicular neoplasm, 11 of cystic change and 3 of inadequate) by FNA, with the results being confirmed histopathologically by operation. Thallium-201 scintigraphy was performed at 15 minutes(early scan) and 2-3 hours(late scan) after the intravenous administration of 37 MBq of thallium-201. Malignant nodules were defined by the retention of Thallium-201 on delayed images. RESULTS: In the 43 patients with inconclusive FNA diagnosis, Thallium-201 scan had a sensitivity of 75.0%, specificity of 62.9% and accuracy of 65.1%. The positive and negative predictive values were 31.6% and 91.7%, respectively. In the 29 patients with follicular neoplasm by FNA, Thallium-201 scan had a sensitivity of 83.3%, specificity of 60.9% and accuracy of 65.5%. The positive and negative predictive values were 35.7% and 93.3%, respectively. CONCLUSION: In particular, Thallium-201 scintigraphy demonstrated a high negative predictive value, Therefore, for patients with inconclusive FNA findings, Thallium-201 scintigraphy might be useful in differentiating between benign and malignant thyroid nodules, and has the potential to reduce the rate of unnecessary operations in benign nodules.


 KES
KES

 First
First Prev
Prev



